A stroke occurs when blood flow to a part of the brain is suddenly interrupted, preventing brain cells from receiving oxygen and nutrients. It is a medical emergency, as brain cells can begin to die within minutes if the blood supply is not restored. Without immediate treatment, a stroke can lead to long-term disability, serious complications, or even death. Globally, stroke is one of the leading causes of death and disability, with about 11.9 million new cases each year and a high lifetime risk for adults (WHO). This page explains stroke in detail, including its causes, warning signs, diagnosis, treatment options, prevention, and recovery.
A stroke is a sudden condition that occurs when blood flow to a part of the brain is reduced or completely blocked, stopping brain cells from receiving oxygen and nutrients. It is also commonly called a brain attack or cerebrovascular accident (CVA). Because the brain relies on a constant blood supply, even a brief interruption can cause damage, which is why strokes often happen suddenly and without warning.
A stroke is a medical emergency because brain cells begin to die within minutes when deprived of oxygen — a concept often described as *“time is brain.” Any delay in treatment increases the risk of permanent brain damage, long-term disability, or death. Quick action and immediate contact with emergency services at the first sign of symptoms can significantly improve survival and recovery outcomes.
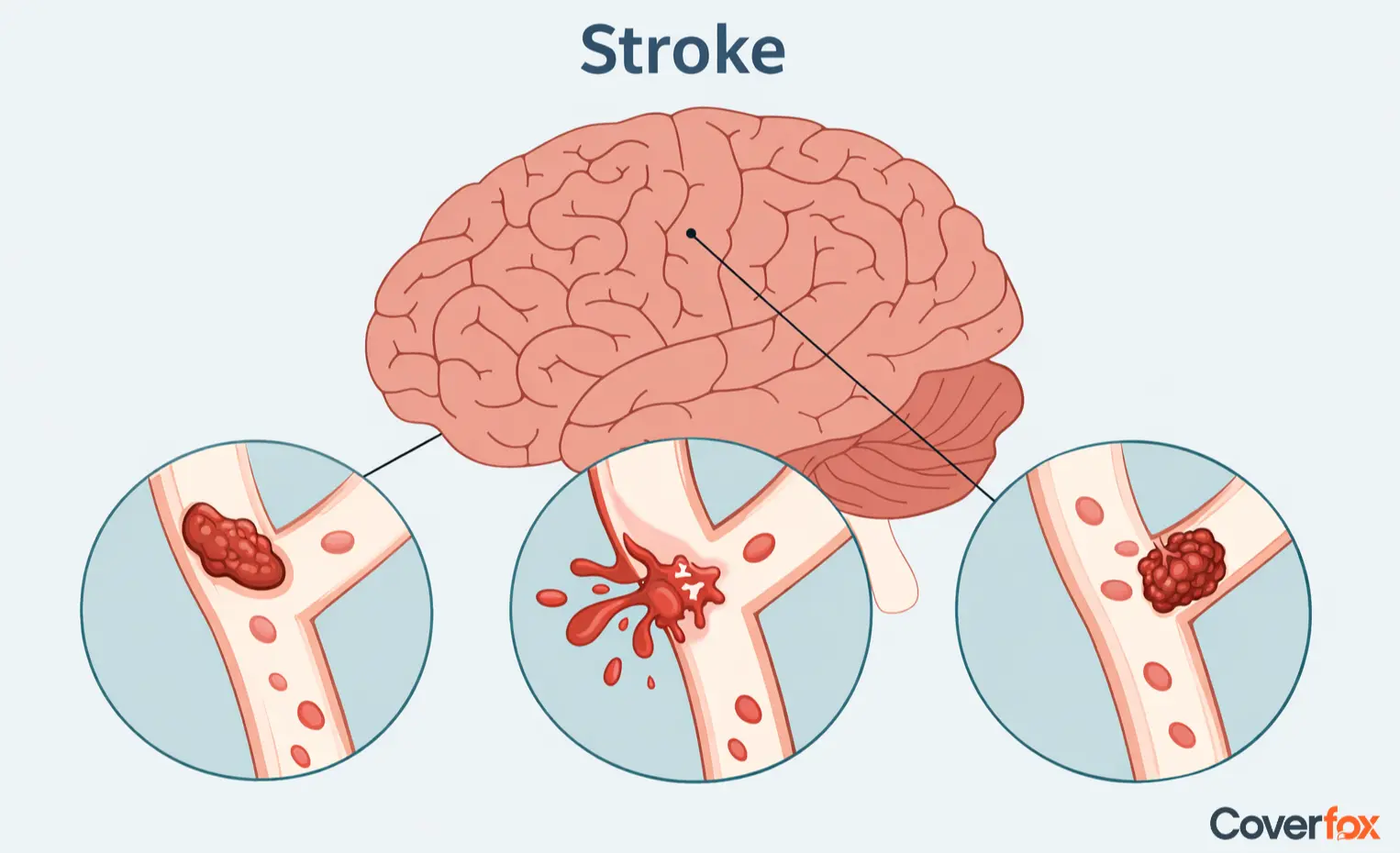
Strokes are classified based on what disrupts blood flow to the brain, either a blockage, bleeding, or a temporary interruption. Understanding the different types helps explain how strokes occur and why their risks and outcomes can vary.
An ischaemic stroke occurs when a blood clot blocks an artery supplying the brain, reducing oxygen and nutrient delivery to brain tissue.
It happens when a clot forms in an artery that supplies blood to the brain, often due to plaque buildup (atherosclerosis).
It occurs when a clot forms elsewhere, commonly in the heart due to atrial fibrillation and travels to the brain. Conditions like carotid artery disease and narrowed blood vessels increase the risk by limiting oxygen supply to brain cells.
A haemorrhagic stroke happens when a blood vessel in the brain ruptures and bleeds, increasing pressure on brain tissue and causing damage.
This involves bleeding directly into the brain tissue, often linked to long-standing high blood pressure.
This occurs when bleeding happens in the space around the brain, commonly due to a ruptured aneurysm. Other risk factors include arteriovenous malformations (AVMs), weakened blood vessels, use of blood-thinning medications, and head injury.
A TIA, often called a mini-stroke, is caused by a temporary blockage that produces stroke-like symptoms but resolves within minutes or hours. Although symptoms disappear, a TIA is a serious warning sign and indicates a high risk of a future major stroke. Emergency medical evaluation is essential, even if the person feels better.
The BE FAST framework is an easy way to recognise the most common warning signs of a stroke. Stroke symptoms usually appear suddenly, are often painless, and worsen quickly if treatment is delayed.
Sudden loss of balance, dizziness, or difficulty walking
Sudden trouble seeing in one or both eyes, blurred or double vision
One side of the face droops or feels numb; an uneven smile
Weakness or numbness in one arm (or leg), difficulty lifting it
Slurred speech, difficulty speaking, or trouble understanding words
Time is critical! Call emergency services immediately if any of these signs appear.
Delaying care increases brain damage, as brain cells begin dying within minutes without oxygen.
Some stroke symptoms may not fit neatly into the BE FAST checklist but are equally serious and require urgent attention.
Sudden, severe headache with no known cause (more common in haemorrhagic stroke)
Confusion, disorientation, or difficulty understanding simple instructions
Sudden vision loss or visual field defects
Difficulty swallowing (choking or drooling)
Seizures without a prior history
Sudden paralysis or numbness on one side of the body
Memory problems or sudden personality or behaviour changes
Nausea or vomiting not linked to food or illness
Poor coordination or inability to perform simple movements
A stroke occurs when blood flow to the brain is disrupted, either by a blockage or by bleeding. Several underlying conditions and triggers can lead to this interruption.
Blood clots that block arteries supplying the brain
Plaque buildup (atherosclerosis) that narrows blood vessels and reduces blood flow
Rupture of weakened blood vessels, leading to bleeding in or around the brain
Heart conditions, such as atrial fibrillation, that allow clots to form and travel to the brain
Long-standing high blood pressure, which damages and weakens blood vessels
Bleeding disorders or abnormalities in blood clotting
Medication-related bleeding, especially from blood thinners, when not properly monitored
Stroke risk depends on a combination of modifiable (controllable) and non-modifiable (non-controllable) factors.
High blood pressure (the leading risk factor for stroke)
Diabetes
Smoking and tobacco use
Obesity and physical inactivity
High cholesterol levels
Excessive alcohol consumption
Use of recreational drugs (such as cocaine or amphetamines)
Poor sleep and sleep apnoea
Unhealthy diet and chronic stress
Exposure to air pollution over time
Increasing age, especially over 55
Family history or genetic predisposition
Male sex (higher risk), though women often have more severe outcomes
Pregnancy and pregnancy-related conditions
Existing heart disease or prior stroke
Stroke diagnosis focuses on speed and accuracy, as early confirmation allows timely, life-saving treatment.
Doctors assess symptoms, onset time, medical history, and perform a neurological exam to check speech, movement, vision, and reflexes.
A CT scan or MRI is done urgently to confirm a stroke and determine whether it is caused by a blockage or bleeding.
These help check blood sugar, clotting ability, infection, and other conditions that may mimic or worsen stroke.
ECG, echocardiogram, carotid ultrasound, or CT/MR angiography may be used to identify heart rhythm problems or narrowed blood vessels.
Lumbar puncture or advanced imaging may be done in complex or unclear cases.
Emergency treatment for stroke focuses on saving brain tissue and preventing further damage. The primary goals are to restore blood flow in blocked strokes or stop bleeding in haemorrhagic strokes, while stabilising vital functions such as breathing, blood pressure, and blood sugar. Rapid brain imaging guides doctors in choosing the right treatment without delay.
Specialised stroke unit care plays a crucial role, as these units are equipped with trained teams, continuous monitoring, and protocols designed specifically for stroke management. Early treatment in a stroke unit significantly reduces complications, disability, and the risk of death.
Treatment for ischaemic stroke aims to quickly restore blood flow to the brain and prevent further clot formation, as every minute of delay increases brain damage.
Medications such as tissue plasminogen activator (tPA) are given through a vein to dissolve the clot blocking blood flow. These drugs are most effective when administered within a strict time window after symptom onset and require careful evaluation to reduce bleeding risk.
For large clots, doctors may perform a minimally invasive procedure where a catheter is guided through a blood vessel to physically remove the clot from the brain artery. This treatment can significantly improve outcomes when done quickly in eligible patients.
Medicines like aspirin or blood thinners are used after the acute phase to prevent new clots from forming, especially in patients with conditions such as atrial fibrillation.
Treatment for haemorrhagic stroke focuses on stopping the bleeding, reducing pressure on the brain, and preventing further damage. Management depends on the location and severity of the bleed.
Immediate care includes controlling blood pressure, maintaining oxygen levels, and closely monitoring neurological status to prevent worsening brain injury.
If the patient is taking anticoagulants or antiplatelet drugs, specific medications or blood products may be given to reverse their effects and limit further bleeding.
Surgery may be required to remove accumulated blood, relieve pressure on the brain, or repair damaged blood vessels. Procedures can include clipping or coiling of aneurysms or removing abnormal vessels such as arteriovenous malformations (AVMs).
Medications and supportive measures are used to reduce intracranial pressure and prevent complications like brain herniation.
Care in a specialised stroke unit or intensive care unit allows continuous monitoring and rapid response to changes in the patient’s condition.
Stroke prevention focuses on reducing risk factors that damage blood vessels and increase clot formation.
Control blood pressure, as hypertension is the leading cause of stroke.
Quit smoking and avoid tobacco in all forms.
Follow a healthy, balanced diet low in salt, sugar, and unhealthy fats.
Exercise regularly to maintain a healthy weight and improve circulation.
Manage diabetes and cholesterol with medication and lifestyle changes.
Limit alcohol intake and avoid recreational drugs.
Go for regular medical check-ups to detect and manage risk factors early.
After a stroke or TIA, secondary prevention is critical to reduce the risk of recurrence.
Antiplatelet medicines (such as aspirin) to prevent clot formation.
Anticoagulants for patients with atrial fibrillation or other heart rhythm disorders.
Statins to lower cholesterol and stabilise plaque in blood vessels.
Carotid artery treatments (surgery or stenting) if significant narrowing is present.
Strict control of blood pressure, blood sugar, and cholesterol levels.
Long-term management of heart rhythm disorders and adherence to prescribed medications.
Stroke rehabilitation helps survivors regain function and independence through physical, occupational, speech, and cognitive therapy, along with psychological support. Rehabilitation usually starts early and focuses on improving movement, communication, daily activities, and emotional well-being. Recovery timelines vary widely—from weeks to months or longer, depending on stroke severity, affected brain areas, and overall health.
Life after a stroke may involve lasting physical, cognitive, and emotional changes that require ongoing care and support.
Mobility issues such as weakness, paralysis, or balance problems.
Speech and communication difficulties.
Memory loss, reduced concentration, or problem-solving challenges.
Emotional changes, depression, anxiety, or mood swings.
Need for long-term rehabilitation, regular follow-up care, and strong family or caregiver support.
After a stroke, you may experience short- or long-term complications that affect daily life, but many can be managed with the right care and support.
Difficulty walking, weakness, or paralysis on one side of the body.
Problems with speech, understanding, or swallowing.
Memory loss, confusion, or trouble concentrating.
Emotional changes such as depression, anxiety, or irritability.
Chronic pain, muscle stiffness, or spasms.
Increased risk of infections, falls, or another stroke.
Dependence on others for daily activities and self-care.
Stroke risk and management can differ in certain groups due to unique physiological changes, existing medical conditions, or age-related factors.
Stroke during pregnancy or the postpartum period is rare but serious. Risk increases due to hormonal changes, high blood pressure, pre-eclampsia, and clotting disorders. Early recognition and coordinated care between obstetricians and neurologists are essential for the safety of both mother and baby.
Stroke risk rises significantly with age due to long-standing conditions such as hypertension, diabetes, and atherosclerosis. Recovery may take longer, and rehabilitation often needs to be tailored to address frailty, mobility issues, and cognitive decline.
Individuals with heart diseases like atrial fibrillation or heart failure have a higher risk of clot-related strokes. Chronic kidney disease increases stroke risk due to blood pressure imbalance and vascular damage, requiring careful medication management and close medical follow-up.
You should call emergency services immediately if you or someone else shows sudden signs of stroke, such as face drooping, arm weakness, speech difficulty, vision problems, or loss of balance (BE FAST). Even if symptoms improve or disappear, urgent medical attention is critical. Acting fast can save brain cells, reduce disability, and save lives.
Yes, stroke is generally covered under most health insurance policies in India, as it is treated as a medical emergency. Coverage usually includes hospitalisation expenses, ICU charges, diagnostic tests (CT/MRI), doctor’s fees, surgeries if required, and medications during hospital stay. Many policies also cover post-hospitalisation care and rehabilitation, though terms, sub-limits, and waiting periods may apply as per policy conditions. And opting for critical illness cover further ensures you get the full treatment covered.
Disclaimer: The information provided above is for general awareness and educational purposes only. It should not be considered a substitute for professional medical advice, diagnosis, or treatment.
Yes, stroke can occur at any age due to factors like heart conditions, blood disorders, lifestyle habits, or genetic risks.
No, many people survive a stroke, especially with early treatment, though recovery and outcomes vary.
Some symptoms may resolve temporarily (as in a TIA), but this is still a medical emergency and needs urgent evaluation.
Recovery can take weeks, months, or longer, depending on stroke severity, treatment timing, and rehabilitation.
Yes, strokes can occur during sleep and may be noticed upon waking, often called a “wake-up stroke.”
Stroke itself is not directly inherited, but genetic factors can increase risk through conditions like hypertension or diabetes.
A massive stroke refers to extensive brain damage due to a large blockage or bleed and often causes severe disability.
Not always, but managing risk factors like blood pressure, smoking, and diabetes greatly reduces risk.
The most common cause is blocked blood vessels due to clots, often linked to high blood pressure and heart disease.
Face drooping, arm weakness, speech difficulty, vision problems, and loss of balance or coordination.
Yes, some strokes occur suddenly with little or no warning, which is why awareness is critical.
The event itself is sudden, but its effects can last from a short time to lifelong, depending on damage.
A stroke causes lasting brain damage, while a TIA causes temporary symptoms but signals high future stroke risk.
A stroke usually affects the opposite side of the body from the area of the brain involved.
Yes, though rare, strokes can occur in young adults and children due to specific medical conditions.
In many health and critical illness plans, stroke is covered, subject to policy terms and definitions, and guidelines set by IRDAI.



























